Do You Really Need More Medicare Advantage? Here’s the Truth About Your 2026 Payer Mix
Medicare Advantage is taking over the market in 2026, but is it killing your agency's value? This guide breaks down why higher MA enrollment can lead to lower valuation multiples and more administrative headaches for owners. Learn how to balance your payer mix and prepare for a high-value exit despite the shifting regulatory landscape.
5/11/20264 min read


Valuation Math: The Cost of Being MA-Dependent
Let’s look at a concrete example. Imagine two home health or hospice agencies, both generating 1 million dollars in EBITDA (Earnings Before Interest, Taxes, Depreciation, and Amortization).
Agency A has a 90 percent Traditional Medicare mix. Because this revenue is predictable and has lower administrative costs, a buyer might value this agency at a 6x multiple. The sale price would be 6 million dollars.
Agency B has a 60 percent Medicare Advantage mix. Because the revenue is at the mercy of private insurers who can change their auth requirements or rates at any time, a buyer might see this as a higher risk. They might apply a 4x multiple. The sale price for the same 1 million dollars in profit is now only 4 million dollars.
By leaning too heavily into MA without a clear strategy, you could be leaving 2 million dollars on the table when you decide to sell your business.
The Medicare Advantage Trap in 2026
The "trap" is simple. The volume is tempting. With MA enrollment growing, it is the easiest way to grow your census. But more volume does not always mean more profit.
Many owners find themselves in a cycle where they have to hire more back-office help just to manage the paperwork for the MA plans. This erodes the small margins these plans provide. In 2026, the administrative burden has reached a boiling point. The time spent waiting for a prior authorization to be approved is time your clinicians are not in the field, and it is time your patients are not receiving care.
Payer Mix Comparison for Home Health or Hospice Owners
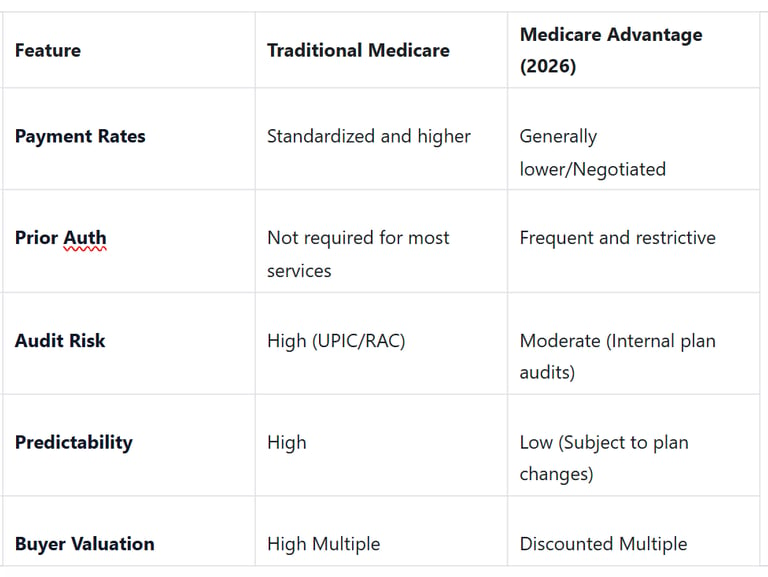
Owner Vignette: The Florida Squeeze
Consider Sarah, an owner of a mid-sized hospice agency in Florida. For years, she focused solely on Traditional Medicare. As the local market shifted, her referral sources started sending more MA patients. To keep her referral partners happy, she signed contracts with three major MA plans.
Within a year, her census was 40 percent Medicare Advantage. Sarah was busier than ever, but her bank account did not show it. She had to hire two full-time "authorization coordinators" to handle the constant denials. When she approached us to discuss a potential sale, she was shocked to learn that her valuation was lower than it would have been two years ago. The increased "noise" in her financials from the MA contracts made her business harder to underwrite.
The 2026 MA Final Rule: A Silver Lining?
It is not all bad news. The 2026 MA Final Rule has introduced some much-needed protections. One of the biggest wins is the push for continuity of care. The rule now makes it harder for MA plans to abruptly cut off services when a patient transitions from a hospital to a home health or hospice setting.
These protections are designed to ensure that if a plan has already authorized a course of treatment, they cannot easily backtrack. For you, this means a bit more stability in your revenue cycle. It is a step toward making MA patients look a little more like Traditional Medicare patients in terms of care consistency.
Plain-Language Glossary
EBITDA: A measure of your agency's operating performance. It is essentially your profit before accounting for interest, taxes, and non-cash items.
Multiple: The number a buyer multiplies your EBITDA by to determine the purchase price.
Prior Authorization: A requirement by an insurance plan that your agency gets permission before providing a specific service to get paid.
Payer Mix: The percentage of your total revenue that comes from different sources like Medicare, Medicaid, and private insurance.
VBC (Value-Based Care): A payment model where providers are paid based on patient health outcomes rather than just the number of services provided.


Strategic Advice: Don't Just Play, Play to Win
If you are going to take on more Medicare Advantage, you have to be strategic about it. You cannot just sign every contract that comes across your desk.
Selective Contracting: Look for plans that are moving toward Value-Based Care (VBC) models. These plans often offer higher rates or bonus structures for agencies that can prove they reduce hospital readmissions.
Diversification: Never let one MA plan represent more than 15 percent of your total revenue. This reduces your risk if that plan decides to change their reimbursement structure.
Invest in Tech: Use software that automates the prior authorization process. If you can lower the human cost of managing these plans, you can protect your margins.
Exit Timing and the 2026 Window
As the market continues to consolidate, the window for achieving a peak valuation is narrowing. Buyers are becoming more sophisticated in how they look at your data. In 2026, we are not just looking at your patient count. We are looking at your clinical outcomes and your payer stability.
If your agency is currently 80 percent Traditional Medicare, you are in a "sweet spot" for a high-valuation exit. If you are starting to see that number slip toward 50 percent, now might be the time to evaluate a partnership or sale before your multiple is compressed by the weight of Medicare Advantage.
So what should you do now?
Audit your current payer mix: Calculate exactly what percentage of your profit (not just revenue) comes from each payer.
Review your MA contracts: Identify which plans have the highest denial rates and consider dropping the ones that cost you more in admin time than they pay in clinical care.
Focus on VBC metrics: Start tracking your readmission rates and patient satisfaction scores religiously. This data makes your MA volume more attractive to buyers.
Reach out for a valuation check: Even if you are not ready to sell today, knowing how a buyer like Senate Healthcare views your current mix can help you course-correct for a future exit.
At Senate Healthcare, we are actively looking to acquire home health or hospice agencies that have a strong clinical foundation. We understand the pressures of the 2026 regulatory environment because we are operators too. We are not brokers or advisors. We are buyers looking to partner with owners who want to secure their legacy and achieve a fair valuation for the business they have spent years building. If you are ready to explore what a transition looks like, let’s talk.
Unlock Your 30-Minute Agency Succession Review
Maybe you're ready to expand your reach, or perhaps it's time to consider your legacy and the future of your business. Either way, it all begins with a conversation. Schedule a confidential, no-obligation call to explore what the future might hold for you and your business.
Complete the form, and we'll reach out for a chat...


© 2025 SENATE HEALTHCARE LLC.
ALL RIGHTS RESERVED

