7 Compliance Mistakes You’re Making with Provider Enrollment (and How They Kill Your Deal)
Is your home health or hospice enrollment a "silent deal killer"? Many owners ignore PECOS and IRS data mismatches until they try to sell, only to find their valuation plummeting. This post breaks down the 7 most common compliance mistakes that lead to "valuation haircuts" and how to fix them before you hit the market.
4/22/20266 min read


Quick-Scan Summary
Who this is for: Home health or hospice owners planning to sell their agency within the next 12 to 24 months.
Key Takeaways:
Provider enrollment is no longer just a back-office chore; it is a primary focus of buyer due diligence.
Minor discrepancies in PECOS or IRS data can lead to retroactive payment revocations.
Cleaning up your enrollment data before a sale can prevent significant "valuation haircuts" or deal delays.
Every home health or hospice owner knows the pain of a Medicare survey. You prepare for weeks, check every chart, and hold your breath until the exit interview. But there is a quieter, more insidious threat to your business that many owners ignore until it is too late: provider enrollment.
In the world of M&A, enrollment is often the "silent deal killer." You can have a perfect clinical record and a growing census, but if your PECOS (Provider Enrollment, Chain, and Ownership System) records are a mess, a buyer like Senate Healthcare will see a massive red flag. When we look to acquire an agency, we are not just buying your patient list; we are buying your right to get paid by the government. If that right is on shaky ground due to administrative sloppiness, the deal either slows down or the price goes down.
In 2026, the stakes are higher than ever. CMS has shifted toward a more aggressive stance on "retroactive revocations," where they can pull back payments if they find your enrollment data was inaccurate during the time services were rendered. For an owner looking to exit, this is a nightmare.


The 7 Enrollment Mistakes Killing Your Exit Value
1. The IRS Name Mismatch (The Identity Crisis)
This is the most common and arguably the silliest mistake we see. Your name in the PECOS system must exactly match the name associated with your Tax Identification Number (TIN) at the IRS. If your IRS letter (CP-575) says "Home Health of Springfield LLC" and your PECOS filing says "Springfield Home Health," you have a problem.
During due diligence, if a buyer finds a mismatch, they see a "billing block" risk. If CMS decides to validate your data and finds a discrepancy, they can suspend your payments until it is fixed. For a small agency, a 60-day payment suspension is often a death sentence.
2. The PO Box Trap
CMS requires a physical site address where you provide services or conduct business. Many owners, especially those who started small or work in rural areas, use a PO box or a virtual office for mail. While that might be fine for your marketing flyers, it is a compliance violation for enrollment.
The 2026 regulatory environment is particularly harsh on "shell" locations. If your listed site address is a UPS Store, CMS can revoke your billing privileges immediately. As a buyer, we look for physical site verification because we cannot risk acquiring a "provider to nowhere."
3. Non-Original or Non-Compliant Signatures
We live in a digital world, but CMS still has very specific rules about who can sign enrollment documents and how. Using a digital signature that does not meet NIST standards or having an unauthorized administrative assistant sign "per" the owner can trigger a rejection.
When Senate Healthcare evaluates an acquisition, we review the authorized and delegated officials listed in PECOS. If the person who signed the last update is no longer with the company, the record is technically invalid.
4. The 36-Month Rule Speed Bump
For home health agencies, the "36-Month Rule" is a major hurdle in acquisitions. Under 42 CFR § 424.550(b), if an owner sells an agency that has been in operation for less than 36 months, the provider agreement might not transfer to the buyer. Instead, the agency must undergo a new initial survey.
Owners often try to "game" this by changing ownership percentages slowly. However, savvy buyers will spot this a mile away. If you are at month 30 and want to sell, you need to understand that the "36-month clock" is the most important metric in your valuation.
5. Missing the 30/90 Day Reporting Deadlines
You are required to report changes in ownership, "key person" changes, or site moves within 30 or 90 days, depending on the change. Many owners wait until their revalidation cycle to update this information.
This is a mistake. If we find that your Clinical Director left six months ago and you never updated PECOS, we wonder what else you have forgotten to report. In 2026, CMS is using automated data cross-checks to find these gaps. Failure to report timely is now a ground for revocation.
6. Inconsistent Data Across the "Holy Trinity"
Your data must be consistent across three platforms: PECOS, the National Plan and Provider Enumeration System (NPPES), and your state licensing board. If your license says one thing and your NPI record says another, it creates a "data ghost" that can haunt your billing.
In a sale scenario, inconsistent data leads to "holdbacks." A buyer might hold 20% of the purchase price in escrow for a year just to make sure no enrollment-related audits pop up. That is your money sitting in a bank account instead of your retirement fund.
7. The "Skeleton in the Closet" (Adverse Actions)
Did you have a small fine from the OIG ten years ago? Did a former partner have a license suspension in another state? You must disclose "adverse actions" in your enrollment updates.
Many owners think, "It was a long time ago, and it was minor." But if a buyer finds an undisclosed adverse action during a background check, the trust is broken. Worse, if CMS finds it, they can revoke your current billing privileges for "providing misleading information."


The "Valuation Haircut" Scenario
Let’s look at the math. Suppose you have a hospice agency with $1 million in EBITDA (Earnings Before Interest, Taxes, Depreciation, and Amortization). In a clean deal, you might be looking at a 5x multiple, resulting in a $5 million valuation.
During due diligence, Senate Healthcare finds that your enrollment address is a virtual office and you missed a change of ownership reporting deadline two years ago. We now categorize your revenue as "at risk."
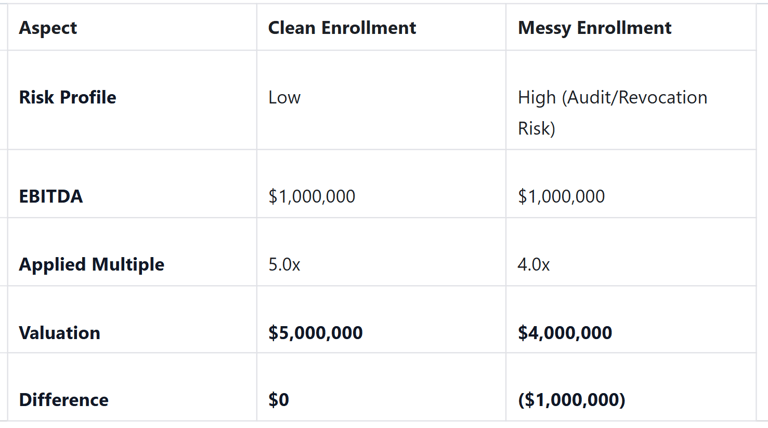
A simple administrative oversight just cost you $1 million at the closing table. This is why we call it the silent deal killer.
The 2026 Insight: Retroactive Revocation
As of late 2025 and into 2026, CMS has increased its use of the "Retroactive Revocation" tool. Previously, if your enrollment was revoked, it usually started the day the letter was sent. Now, if CMS finds you were out of compliance with enrollment rules a year ago, they can move the effective date back.
This means every dollar you collected over the last twelve months could technically be considered an overpayment. No buyer will touch an agency with that kind of exposure without a massive discount or an indemnity that makes the deal unattractive to the seller.


Plain-Language Glossary
PECOS: The online Medicare enrollment system where you tell the government who you are and where you work.
CHOW (Change of Ownership): The process of telling Medicare that a new person or company is taking over the provider agreement.
EBITDA: A measure of your agency's profitability used to determine its sale price.
Multiple: The number (e.g., 4x or 6x) that a buyer multiplies your EBITDA by to get the total purchase price.
Revalidation: The periodic "check-up" where CMS asks you to confirm all your enrollment data is still correct.
So what should you do now?
Perform a "Shadow Audit": Log into PECOS today and compare every line of data against your IRS CP-575 and your state license.
Check Your Signatories: Ensure that the "Authorized Officials" listed in PECOS are actually still in the building and have the authority to sign.
Review the 36-Month Clock: If you have owned the agency for less than three years, consult with a buyer like Senate Healthcare to understand how this affects your exit timing.
Disclose Everything: If there is a "skeleton" in your regulatory closet, it is better to disclose it and explain it than to have a buyer find it in month two of due diligence.
Why Senate Healthcare is Your Partner
We are not brokers or advisors; we are buyers. We are looking to acquire high-quality home health and hospice agencies to join our growing portfolio. Because we are the end-user of your business, we care deeply about the "plumbing" of your enrollment.
When you partner with us, we work with you to identify these administrative risks early. Our goal is a clean, efficient transition that rewards you for the years of hard work you have put into your agency. If you are worried that your "back office" might be holding back your valuation, let's have a conversation.
What has been your biggest headache with PECOS lately? Have you ever had a "name mismatch" hold up a payment? Share your thoughts or reach out to us to talk about how we can help you prepare for a successful exit.
Unlock Your 30-Minute Agency Succession Review
Maybe you're ready to expand your reach, or perhaps it's time to consider your legacy and the future of your business. Either way, it all begins with a conversation. Schedule a confidential, no-obligation call to explore what the future might hold for you and your business.
Complete the form, and we'll reach out for a chat...


© 2025 SENATE HEALTHCARE LLC.
ALL RIGHTS RESERVED

